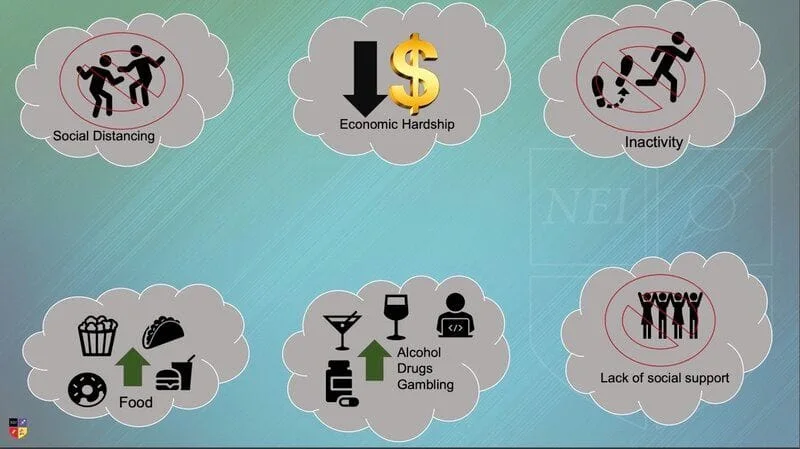
Covid 19 is part of a global syndemic including a public health and mental health crisis.
- The novel coronavirus, SARS-CoV-2 has resulted in significant increases in a variety of mental health issues, such as major depressive disorder, anxiety, and post-traumatic stress disorder
- Factors such as social isolation, malignant uncertainty, high utilization of social media, and loneliness exacerbated physical and mental health conditions
- There are specific populations who are highly vulnerable to the mental health consequences of the pandemic (e.g. high poverty, low social support)
- Suicide rates during the pandemic have risen and can be mitigated by a variety of social programs
- Patients with pre-existing mental health conditions are at higher risk of COVID-19 infection, higher hospitalization rates for COVID-19, and higher COVID-19 related deaths, as well as a reduced response to the COVID-19 vaccine
- Long COVID/Post-COVID-19 Syndrome is a particular concern with possible detrimental effects on mental health and cognition
The perfect storm for mental illness exists:
The COVID-19 global pandemic has resulted in catastrophic, long-lasting mental health consequences.
- The combination of social isolation, lifestyle changes, economic destruction, and job loss has resulted in increased substance use disorders (SUD), family violence, depression, anxiety, and suicide
- Those with pre-existing mental health conditions and/or underlying physical conditions prior to the pandemic are at particularly high risk for exacerbation of psychiatric conditions
- Healthcare workers, especially those on the frontlines working directly with patients affected by the virus are also at high risk for mental health consequences
Brain Fog
Long COVID-19, also known as post-COVID syndrome (PASC), involves a wide range of health problems that occur after recovering from COVID-19 infection. Sometimes, symptoms of PASC can include cognitive difficulties.
Brain fog is not a scientific term; it is used by individuals to describe how they feel when their thinking is sluggish, fuzzy, and not sharp.
Reported problems include:
- Confusion
- Orientation
- Attention
- Concentration
- Memory
- Motor responses
- Visual-spatial skills
Reported struggles with emotional functioning:
- Agitation
- Anxiety
- Depression
- Post-Traumatic Stress Disorder (PTSD)
These symptoms may cause a lack of motivation, frustration with increased feelings of hopelessness, helplessness, depression and anxiety related to their situation. Some people find it quite debilitating.
Brain fog can be a symptom of many other disorders not just a sequala of COVID-19. This is where a root cause analysis approach is critical. Is it related to psychological stressors, disease process or lifestyle?
Brain Fog Evaluation
- COVID-19
- Multisystem Inflammation
- Lack of oxygen secondary to cardiac or pulmonary disease
- Medication
- Oxygenation problems due to lung or cardiac issues
- Inflammation in multiple systems
- Medication side effects
- Sleep disturbance
- Stress, anxiety, media consumption, and/or solitude
Lifestyle
- Poor diet
- Vitamin deficiency ( D, B12)
- Mineral deficiency (iron, iodine)
- Excess sugar and processed foods
- Nutrient deficit
- Substances
- Alcohol
- Marijuana and other drugs
- Change in caffeine or nicotine use
Sleep
Sleep services all aspects of our body including molecular, energy balance, intellectual function, mood and alertness. It affects our growth and stress hormones, immune system, appetite, breathing, blood pressure as well as cardiovascular health.
- Insufficient sleep may simulate brain fog
- Sleep architecture and sleep disorders will affect mental clarity
- Insomnia—lasting at least 3 nights per week for more than a month—can trigger problems such as exhaustion, irritability and difficulty with concentration
Psychology
- Depression and pseudo-dementia may present with impaired concentration, decreased motivation, apathy and struggles with task completion
- Anxiety, stress and trauma heighten emotional exhaustion leading to cognitive impairment
- Narcissistic Injury – unemployment, failure, shame – withdrawal can increase one’s perception of brain fog
Metabolic/Endocrine
- Hypothyroidism and hyperthyroidism are both linked with trouble concentrating, memory issues, and cognitive irregularities
- Diabetes: complications of hyperglycemia and hypoglycemia can produce symptoms of decreased alertness, fogginess, inability to focus.
- Hepatic/Renal dysfunction can cause accumulation of toxins which will present with neurocognitive symptoms.
- Menopause: the decrease in estrogen and progesterone temporarily causes concentration and memory difficulties.
Additional Causes of Brain Fog
- Fibromyalgia (fibro fog)
- Lyme Disease
- Lupus
- Traumatic Brain Injury (TBI)
- Anemia
- Hemodynamic abnormalities
- Chemotherapy “chemo brain”
- Medication side effects
- Ketogenic Diets
There are many considerations that may factor into brain fog. Dr. Singer has the expertise, consultative specialists to determine the root cause of your brain fog and facilitate the best treatment plans for you. Some options may include:
- Accurate diagnosis
- Pharmacotherapy
- Psychotherapy techniques
- Trigger management
- Cognitive rehabilitation
- Executive function coaching
- Resilience and coping strategies
Although there is no universal treatment for these cognitive difficulties, some rehabilitation modalities can retrain the brain to work on the areas that are most challenging.
(Slide credit: Neuroscience Education Institute)